Written by: Compliance blogger
More...
The direct health impacts of pandemics can be catastrophic. Pandemics are large-scale outbreaks of infectious disease that can greatly increase morbidity and mortality over a wide geographic area and cause significant economic, social, and political disruption. The world has and will be suffering through the various stages of the Coronavirus (COVID-19) pandemic for months and perhaps even years to come.
The indirect health impacts of pandemics can increase morbidity and mortality further. Drivers of indirect health impacts include diversion or depletion of resources to provide routine care and the decreased access to routine care resulting from an inability to travel, fear, or other factors. Additionally, fear can also lead to an upsurge of the “worried well” seeking unnecessary care, further burdening the health care system.
The availability of health care workers also decreases during a pandemic because of illness, death, and fear-driven absenteeism. Health care organizations must address organizational risk factors to care for their workforce which, in turn, cares for the health of the community.
Pandemic Intervals Framework
Though most pandemic research and guidance is specific to influenza, the same premises can be applied to the current COVID-19 pandemic. The Pandemic Intervals Framework describes the progression of an influenza pandemic using six intervals:
- Investigation of cases of novel influenza A virus infection in humans;
- Recognition of increased potential for ongoing transmission of a novel influenza A virus;
- Initiation of a pandemic wave;
- Acceleration of a pandemic wave;
- Deceleration of a pandemic wave; and
- Preparation for future pandemic waves.
Occupational Safety and Health Act
The Occupational Safety and Health Act requires employers to comply with safety and health standards and regulations promulgated by OSHA or by a state with an OSHA-approved state plan. In addition, the Act’s General Duty Clause, Section 5(a)(1), requires employers to provide their employees with a workplace free from recognized hazards likely to cause death or serious physical harm.
Please download the OSHA Guidance on Preparing Workplaces for COVID-19 PDF. This guide educates health care administrators on how the virus spreads in the absence of a vaccine and on the results suffered by employers.
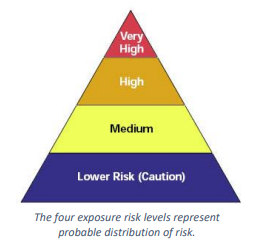
Another OSHA resource is the 1-page Worker Exposure Risk to COVID-19 PDF which helps organizations to classify worker risk of occupational exposure to the virus. Worker risk of occupational exposure to COVID-19 may range from very high to high, medium, or lower (caution) risk.
The level of risk depends in part on the industry, the need for contact with those suspected or known to be infected, and the need for required, repeated contact with persons suspected or known to be infected. To help employers determine appropriate precautions, risk levels are categorized based on four levels:
Centers for Disease Control
The Centers for Disease Control (CDC) has a guidance for businesses which provides employers and workers with recommended SARS-CoV-2 infection prevention strategies to implement in the workplaces. It is highly recommended for all organizations to review: Interim Guidance for Businesses and Employers Responding to Coronavirus Disease 2019 (COVID-19).
Mental PPE: Self-Care Support
The onset of a disaster is often quite sudden. For this reason, even those most prepared may struggle to balance vacillating feelings of fear, stress, anxiety, grief and worry. As unique individuals, our personal feelings will continue to change over time but our ability to adapt using healthy practices will help us to notice and accept how we feel.
The lack of personal protection equipment, or PPE, during this pandemic adds to the mental stress of our health care workforce and other responders. Forward-thinking health care organizations will also consider the “Mental PPE”, or self-care precautions, needed to manage the abrupt changes that are impacting each of our daily lives. With an urgent need to protect ourselves and our families, we depend on our emotional health to help us think clearly and react appropriately to a crisis.
Conclusion
Addressing the safety as well as the physical and mental well-being of our workforce is a huge risk management task that must be addressed. This pandemic is not going away overnight and issues of public health and safety will linger for years to come. Do you want to learn more about COVID-19 and Risk Management in Healthcare Organizations? Go to www.aihc-assn.org for more information.
